HA plays surprising—sometimes contradictory—roles in the immune system.
Did you know that the immune system is the largest and most highly distributed system in your body? The immune system is an amazing organ!
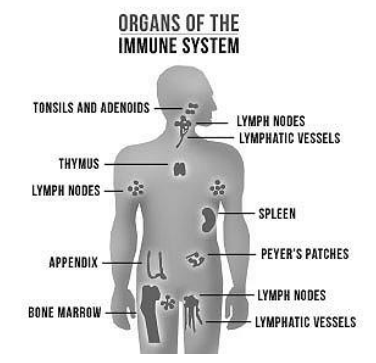
Most organ systems have a specific site in the body that you can point to and say, “There is the heart. It pumps blood through the body.” But the immune system is different. There is not just one organ that defines the immune system because parts and pieces of the immune system occupy many spaces throughout our bodies, including our bone marrow, thymus gland, spleen and lymphatic system and portions of our intestine.
The immune system is the white blood cells and antibody molecules that circulate in the blood to detect and fight off pathogens and other intruders. The immune system is the antibody producing cells that live in the spleen and thymus. The immune system is pockets of immune cells that are clustered in patches spread throughout the lining of the intestine. The immune system is the marrow in the center of bones where new white blood cells are created and mature. Here is what is important: There is solid clinical evidence that all these dispersed parts and pieces of the immune system require Hyaluronic Acid to be healthy and function well.
There are two separate functions in the immune system. The first immune function is innate immunity. The second immune function is adaptive immunity. Innate immunity responds first and quickly to a threat and is a short lasting response. Adaptive immunity responds later and much more slowly to a threat but is a much longer lasting response (Chaplin, 2010). Both kinds of immunity are necessary for health, and both depend on HA to function well. A good way to think of the difference between the two types of
25.
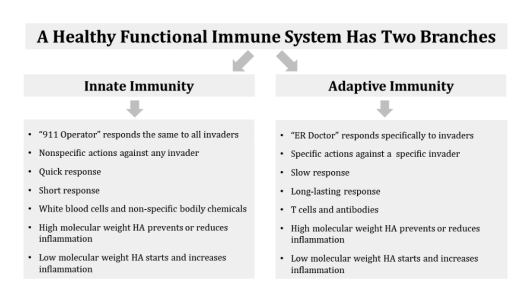
immunity is the differing roles in emergency medicine of 911 operators versus paramedics and emergency room doctors. The innate immune system is the 911 operator who sends an ambulance to anyone who urgently needs to get to the hospital for any reason. The adaptive immune system is the paramedic and the emergency room doctor at the hospital who provide the exact treatment a patient requires to survive the heart attack or severe injury they have experienced.
Hyaluronic Acid in the innate immune system.
The innate immune system’s main weapon against threats to health is inflammation (Cronkite & Strutt, 2018). You might think that inflammation is a result of an infection or other problem: “I got a cut, and it became inflamed.” However, inflammation really is a proactive mechanism the body uses to maintain balance: Inflammation is how the body gets rid of bacteria that could cause the cut to become infected and returns the body to normal. Inflammation is often portrayed as being bad and something to eliminate from your body, but this perception is flawed. Inflammation is an important body defense. It is only when inflammation occurs without reason or runs out of control that it becomes “bad”.
Here is the plot of the innate immune system story: Certain types of white blood cells continuously patrol our bodies looking for intruders. When these cells detect an intruder—like bacteria that have found their way into your cut—they set off an inflammatory cascade that serves to draw additional white blood cells, called neutrophils, to the site of the cut. Neutrophils are amazing little factories that produce and release enzymes and oxidants that can kill and break down bacteria. Neutrophils also release substances that encourage another type of white blood cell, called phagocytes, to come to the site of the cut. The recruited phagocytes eat the degraded bits of bacteria to remove the cause of inflammation from the body (Cronkite & Strutt, 2018; de laMotte & Kessler, 2015; Hato & Dagher, 2014; Kim & de la Motte, 2020).
HA is known to regulate the function of innate immune cells by using several mechanisms. For example, by binding to the surfaces of the white blood cells, HA activates the cells to play their role in immunity (Rayahin, et al., 2015; Safrankova, et al., 2010). One regulatory mechanism that is thought to activate inflammation is that the patrolling white blood cells, after detecting an intruder, release enzymes that degrade high molecular weight HA into small fragments. These small HA fragments appear to act as danger signals that encourage neutrophils and phagocytes to migrate to the wound or infection and to activate these cells to do their jobs (Cyphert, et al., 2015; Rayahin, et al., 2015).
26
HA is also thought to play a role in ending inflammation when inflammation is no longer necessary. After the bacteria in your cut are degraded by neutrophils and the left over bits are eaten by the phagocytes, the reappearance of high molecular weight HA appears

to help to dampen down the inflammation by binding to molecules on the surface of the now-unnecessary white blood cells to cause them to go dormant and die (Chiou, et al., 2018; Cyphert, et al., 2015; Rayahin, et al., 2015).
So, you can see that both high and low molecular weight HA are important in regulating the innate immune system. The trick is to have the right amount of each size of HA in the right ratio at the right time. Having just enough low molecular weight HA at the right time and right place is required to start an innate immune response (Cyphert, et al., 2015; Rayahin, et al., 2015) but having too much low molecular weight HA is known to promote the spread of cancer cells (Kouvidi, et al., 2011). Having just enough high molecular weight HA at the right time and right place is required to stop an innate immune response (Cyphert, et al., 2015; Rayahin, et al., 2015) but having too much high molecular weight HA at the wrong time and in the wrong place is a problem, too. We will discuss an important instance of the detrimental effects of too much high molecular weight HA in a few paragraphs (Shi, et al., 2020).
Also, keep in mind that low molecular weight HA is created by degrading high molecular weight HA into smaller pieces (Gupta, et al., 2019) so not having enough high molecular weight HA indirectly can cause impaired innate immune responses (Cyphert, et al., 2015; Rayahin, et al., 2015). Mostly, we do not need to worry about having the correct balance of the high and low molecular weight HA because, when the human body is healthy, it has very strong mechanisms to govern the production and destruction of HA (Jiang, et al., 2011). Eating a healthy diet and making sure that our bodies have enough high molecular weight HA, such as by taking an oral supplement, is sufficient to support those mechanisms (Cyphert, 2015). However, as we will discuss in a later section, bacteria, viruses, and some non-communicable diseases can subvert this system to cause serious, deadly illness (Mong, 2020; Jiang, 2011).
Hyaluronic Acid in the adaptive immune system.
The other function of the immune system is adaptive immunity (Chaplin, 2010). The adaptive immune response differs from the innate immune response in that the adaptive immune system recognizes specific invaders and mounts a distinct response to each different invaderThe innate immune system does not care if the invader is a bacterium, a virus, or a splinter in your finger; it responds the same to all invaders. Like an emergency room doctor, the adaptive immune system takes the time to recognize that you have been infected with a specific pathogen and additional time to distinguish the chicken pox virus from the strep throat bacterium, for example. Then, the adaptive immune system activates a two-part immune response that involves, first, producing antibodies that specifically bind to and mark the pathogen for destruction and, second, causing cells to mature that specifically destroy the pathogen. The adaptive immune response is slower than the innate immune response due to the necessity to gear up synthesis of the specific antibodies and to create and activate the cells that attack the pathogen. The innate immune response provides just enough short-term, non-specific protection to give the adaptive immune response time to develop specific protection to fight off the invader.
As in the innate immune system, HA plays a role in the adaptive immune system. High molecular weight HA binds to a cell surface molecule on the outside of adaptive immune cells, specifically white blood cells called T lymphocytes (Asari, et al., 2010). T lymphocytes (or “T cells” in medical and research parlance) are the cells that specifically recognize molecules from foreign invaders, distinguish those molecules from molecules that are part of the body, and then activate the adaptive immune response. Binding of HA to T cells helps to regulate and modulate the function of T cells to activate various immune functions, such as causing other immune cells to secrete antibody molecules to specifically target invaders.
27
HA and viral infections.
There is some basic science, but not clinical, evidence that HA can protect cells from being infected with some, but not all, viruses (Cermelli, et al., 2011). Scientists do not quite understand how HA accomplishes this. However, having an understanding of how viruses infect cells offers some insight. 28All viruses infect human cells by binding initially to the surface of cells and then moving inside the cells. Once inside the cells, viruses highjack the cells’ machinery to make more copies of themselves. When a certain number of offspring viruses are produced, the viruses start to exit from cells. In the process, viruses often kill the cells. In cultured cells (not in animals or humans), scientists observed that HA reduced the number of cells that were killed by different types of viruses and that HA was able to reduce the total number of offspring viruses
produced. Scientists think that HA alters cellular function in a way that must interfere with viruses being able to bind to and enter cells or with viruses being able to highjack the cells’ machinery to make more viruses. It does not appear that HA directly interacts with the viruses; rather, it is HA’s effects on the cells that are important (Cermelli, et al., 2011).
28St. John’s Health. Health & Medical Resources. https://www.sjahs.org/virus-life-cycle/
HA, COVID-19, and out-of-control innate immunity.
One problem with the innate immune system and the processes that it uses to fight intruders, such as inflammation, is that it these processes very easily can get out of control (Shi, et al., 2020). Going back to the car analogy at the beginning of the book, an out-of-control innate immune system is like a car speeding down the highway. The driver suddenly needs to stop but discovers that his brakes have failed, perhaps because all the brake fluid has drained out of the car. Bad things are going to happen to that car. Let us just hope that the driver is wearing a seatbelt! There’s evidence that HA might be a component of the “brake fluid” that acts to keep the immune system’s brakes functioning well.
Pathogens, like bacteria and viruses, can cause human disease and death by causing the innate immune system to lose control. The good news is that pathogens that cause the innate immune system to function uncontrollably, most often are not very efficient at spreading between people because they tend to kill patients before they can pass on the pathogen to other people (Engering, et al., 2013). So, while these pathogens do kill the people they infect, they are not transferred efficiently to enough people to cause epidemics (isolated outbreaks of disease) or pandemics (world-wide outbreaks of disease caused by many concurrent epidemics occurring in multiple places). But, every now and then, a scary pathogen emerges that efficiently can be transmitted from one person to many other people and can cause the innate immune system to roar out of control (Boulos & Gareghty, 2020; Mong, et al., 2020; Rothan, et al., 2020; Shi, et al., 2020; Song, et al., 2020). These types of pathogens cause epidemics and pandemics that result in many people becoming sick and dying, and, thus, are important problems for public health to solve.
The 2020 COVID-19 pandemic was caused by such a pathogen, the SARS-CoV-2 virus. SARS-CoV-2 was able to move efficiently from one person to another by air droplets. The virus also had a long incubation period before illness occurred. This allowed people who were infected, but did not know they were infected, to spread the virus to many other people (Boulos & Geraghty, 2020). In some people, SARS-CoV-2 also was able to damage the brakes on the innate immune system, which allowed the immune system to roar out of control (Rothan, et al., 2020). Part of the way by which SARS-CoV-2 damaged the brakes was to interfere with normal synthesis and breakdown of HA (Bell, et al., 2019; Gupta, 2019).
In some, but not all, people who are infected with SARS-CoV-2, the virus causes a dangerous condition called “cytokine storm”(Shi, et al., 2020; Song, et al., 2020; Sun, et al., 2020). In a cytokine storm, the innate immune system loses control over production of cytokines, which are chemicals it uses to fight infection. Cytokines, when produced by the body in just the right quantities and at just the right time, are very effective to help our bodies fight off infection. However, during cytokine storm, extremely large quantities of these chemicals are produced in an unregulated manner, which causes the body to begin to shut down leading to severe, irreparable organ damage (Shi, et al., 2020; Sun, et al., 2020, Song, et al., 2020). Cytokine storms happen very quickly and cause rapid death, sometimes within hours of onset. Often, there is nothing medical professionals can do to stop cytokine storm once it has started. It is always much better to stop cytokine storm before it happens than to treat it after it starts. In some COVID-19 patients, the SARS-CoV-2 virus causes a cytokine storm that leads to a nearly always fatal lung condition called acute respiratory distress syndrome (ARDS). Most deaths that occur in COVID-19 patients result from ARDS (Mong, et al., 2020; Shi, et al., 2020; Sun, et al., 2020, Song, et al., 2020).
If there was ever a doubt about how important HA balance is to the well-being of the body, that doubt should be ended once and for all by the integral role played by HA in COVID-19 ARDS. Elevated high molecular weight HA concentration in the blood was quickly recognized by doctors as a hallmark sign of SARS-CoV-2 infection in patients (Mong, et al., 2020). The elevated levels of HA resulted because some of the cytokines that are overproduced in the SARS-CoV-2-induced cytokine storm unbalance the body’s tight control over HA synthesis and destruction, leading to over-production of high molecular weight HA (Cyphert, et al., 2015; Fallacara, et al., 2018). Over-production of HA results in far too much high molecular weight HA being present in the lungs (Esposito, et al., 2017; Mong, et al., 2020; Shi, et al., 2020; Sun, et al., 2020, Song, et al., 2020). ARDS develops because the high molecular weight HA absorbs water—sometimes up to 1,000 times its weight in water (Jiang, et al, 2011). Ironically, the ability of high molecular weight HA to absorb water is a benefit of HA in the eye, which we will describe in a later section. However, in the lungs, all the water soaked up by the excess HA causes the supporting layer of air sacs to become very thick. Air sacs, or alveoli in medical terms, are where oxygen breathed in from the air moves between the air sac cells and across the supporting layer below the air sac cells into the blood. This process must occur efficiently for adequate oxygen to enter the blood to keep organs healthy. If the supporting layer becomes too

thick and dense with water, as it does in ARDS, oxygen can’t be exchanged efficiently, and the body starts to shut down organs due to damage caused lack of oxygen (Mong, et al., 2020; Shi, et al., 2020, Sun, et al., 2020; Song et al., 2020).
At the time of writing this book (mid-June 2020), it is too early in the SARS-CoV-2 epidemic to describe clinically validated therapies for COVID-19 ARDS that are based on regaining control over HA metabolism. However, at least one group of clinicians who have treated ARDS caused by SARS-CoV-2 suggest that using drugs that inhibit HA synthesis can prevent buildup of excess HA to prevent ARDS from developing or using drugs that increase HA breakdown can destroy excess HA to restore lung function after ARDS has developed (Cantor, 2007; Shi, et al., 2020).
HA’s anti-inflammatory actions in respiratory disease.
In the previous section, we discussed how cytokine storm resulting from infection with the SARS-CoV-2 virus causes the fatal lung disease ARDS, by stimulating the body to overproduce high molecular weight Hyaluronic Acid in the support layer of the air sacs in the lungs. This is an example of how unregulated synthesis of HA in the body causes disease. In adults with chronic obstructive pulmonary disease (COPD), more HA of unknown molecular weight appeared in the blood in adults experiencing severe COPD attacks compared to adults not experiencing severe COPD attacks (Papakonstantinou, et al., 2019). It is unfortunate that the authors did not test the molecular weight of the HA because molecular weight is known to be important to HA’s functions in the immune system. However, given what we have already read, we might hypothesize that the observed excess HA could be low molecular weight HA, which has been shown in other studies to contribute to inflammation.
If low molecular weight HA increases inflammation, it stands to reason that adding high molecular weight HA, which is anti-inflammatory (Garantziotis, et al., 2016a), to the airway might have the opposite effect to reduce airway inflammation. In fact, clinicians have observed that this is true (Cantor, 2007). In a laboratory model of bacterial pneumonia, isolated human lung cells were infected with bacteria (to mimic bacterial pneumonia). Treating the cultured human lung cells with high molecular weight HA reduced signs of inflammation (Garantziotis & Matalon, 2019; Liu, et al., 2019). Bronchitis patients who were injected with high molecular weight HA got fewer repeat infections (Venge, et al., 1996). In mice with chemically induced, asthma-like lung injuries, high molecular weight HA prevented the immune reaction leading to the asthma-like condition (Lazrak, et al., 2015). In an animal model of lung transplant, low molecular weight HA caused an immune reaction like the immune reaction that causes humans to reject transplanted lungs. Treating the mice with high molecular weight HA prevented the immune reaction that led to rejection of the transplanted lungs and the mice were able to continue to live (Todd, et al., 2014). Unfortunately, many researchers appear to be unaware of the apparent link between molecular weight of HA and its pro or anti-inflammatory effects because many researchers do not describe the molecular weight of the HA used or detected in their studies.
In the next section, we will discuss HA in the gastrointestinal system. Surprisingly, the most important role of HA in the gut is HA’s effect on the immune system. At the beginning of this section, we mentioned that part of the immune system occurred in patches distributed throughout the gut. Well, it turns out that the immune cells in those patches have wide-reaching effects throughout our body—the so called gut-skin-brain axis.
